This month we’re kicking off a new blog series here at Laurel Dental! Every other month through 2019 we will be highlighting a different autoimmune disease and the impacts it has on oral health, and vice versa. Autoimmune diseases are wide ranging diseases that affect many systems of the body. Their commonality though, is that the body begins attacking its own cells wreaking havoc and causing painful and sometimes debilitating symptoms.
Over 23.5 million people in the United States alone suffer from at least one autoimmune disease. These diseases are seen more often in women than in men, and it is hypothesized that hormonal changes may play a role. We’ll be starting the series off this month taking a look at the impact of Rheumatoid Arthritis (RA) on oral health.
Rheumatoid arthritis occurs when your immune system attacks the synovium — the lining of the membranes that surround your joints.The resulting inflammation thickens the synovium, which can eventually destroy the cartilage and bone within the joint. The tendons and ligaments that hold the joint together weaken and stretch.
Gradually, the joint loses its shape and alignment. Rheumatoid arthritis can occur at any age, but it most commonly begins in middle age. People — especially women age 55 and younger — who are overweight or obese appear to be at a somewhat higher risk of developing rheumatoid arthritis.
Possible Links
There are a couple of different hypotheses currently out there as to why so many individuals with RA also suffer from periodontal disease. One such hypothesis is an easy link to make. RA can cause severe pain and stiffness in any of the body’s joints.
Painful hands with limited mobility makes common homecare, such as brushing and flossing much more difficult. If RA also affects the TMJ, this can limit the patient’s ability to open, which further complicates keeping their teeth clean.
A lack of good homecare can certainly increase one’s risk for developing periodontal disease. Poor homecare may not be the exact link, but it is certainly a risk factor shared between the two diseases.
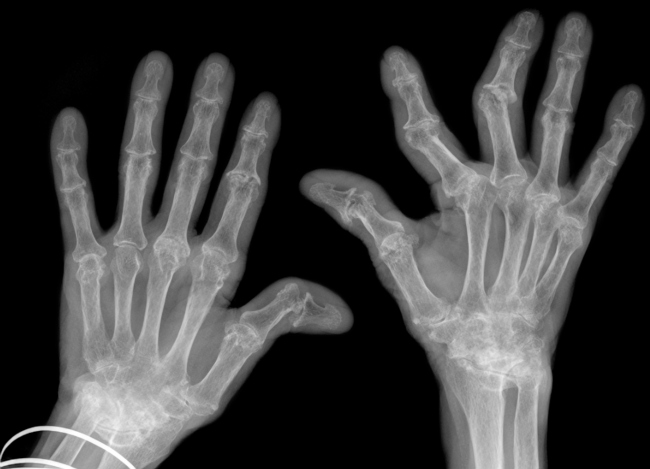
8 times more likely to develop periodontal disease
A German study in 2008 found that patients with RA were 8 times more likely to develop periodontal disease and also noted that poor oral hygiene alone did not explain such a significant increase in risk. This of course leads us to look deeper into the cellular level of disease.
Similarities have been found in oral tissue with periodontal disease and joints with RA. As we well know, the inflammation of periodontal disease causes destruction of the bone and tissue surrounding the teeth. Inflammation is also what causes the breakdown of joints, and pain associated with RA.
Many of the same proinflammatory proteins were found in both diseases (Tumor Necrosis Factor (TNF), Interleukin-1, and Interleukin-6). A different study from Israel also found that genetics may play a role in elevated risk for RA. Cigarette smoking increases your risk of development, particularly if you have a genetic predisposition for developing the disease. Smoking also appears to be associated with greater disease severity.
All of this information and more has led to a better understanding of the entire disease process. One of the early markers of RA is the increase of antibodies to citrullinated peptides. Citrullination is the scientific term, for a change in cell structure that leads it to be seen as a foreign entity to the body.
This citrullination leads the body to release anti-cyclic citrullinated (anti-CCP) antibodies. These antibodies then attack the cells thought to be foreign, even though they are in fact cells of the body. The importance to periodontal disease comes through a link in bacteria.
It was found that at least one strain of bacteria commonly associated with periodontal disease causes the process of citrullination. A study in 2009 concluded that due to these facts, certain oral bacteria could be the cause of RA and/or that periodontal disease may be inducing the disease process of RA.
Treatment
The first thing to do is to get a diagnosis from your physician to build a treatment plan that will best accommodate your needs. A diagnosis can be difficult to determine in the early stages because there is no one blood test or physical finding to confirm.
During a physical exam, your doctor will check your joints for swelling, redness and warmth. He or she may also check your reflexes and muscle strength. People with RA often have an elevated erythrocyte sedimentation rate (ESR, or sed rate) or C-reactive protein (CRP), which may indicate the presence of an inflammatory process in the body.
Other common blood tests look for rheumatoid factor and anti-cyclic citrullinated peptide (anti-CCP) antibodies. Your doctor may also recommend X-rays to help track the progression of rheumatoid arthritis in your joints over time. MRI and ultrasound tests can help your doctor determine the severity of the disease in your body.
When it comes to RA, at this time, there is no discovered cure. But clinical studies indicate that remission of symptoms is more likely when treatment begins early with medications known as disease-modifying antirheumatic drugs (DMARDs).
One can assume then that with all of this information, periodontal disease and rheumatoid arthritis are clearly linked. One of the best ways to control them is to be sure to treat each disease.
If you are suffering from uncontrolled periodontal disease you will likely benefit from scaling and root planing to bring it under control and maintain better oral health with frequent dental visits.
It is also important to work with your physician to control your RA. If you suffer from RA and have a difficult time with you homecare due to stiff or painful joints, speak with your hygienist. You may benefit from different dental tools, including an electric toothbrush or water flosser.
We strive to work closely with our patients’ physicians to care for your entire health. If you have RA, it is imperative to maintain good homecare and frequent visits with your hygienist. We look forward to highlighting other autoimmune diseases over the coming months.
They are not spoken about often, taking a backseat to Smoking and Diabetes when it comes to periodontal disease. It is our hope that continued studies will be done to further understand the etiology of these elusive diseases. If you know someone with RA, please share this link with them!
References:
Arthritis Foundation – https://www.arthritis.org/living-with-arthritis/comorbidities/gum-disease/ra-and-gum-disease.php
Johns Hopkins Arthritis Center – https://www.hopkinsarthritis.org/arthritis-news/5-dental-tips-for-the-ra-patient/
Colgate – https://www.colgate.com/en-us/oral-health/conditions/immune-disorders/ada-06-rheumatoid-arthritis-and-gum-disease-risk
National Library of Medicine, National Institutes of Health – https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4495574/